What if one of the biggest clues about healthy aging is hiding behind your breastbone? Two new studies suggest the thymus, a small immune organ many of us stop thinking about after childhood, may still matter a lot in adulthood.
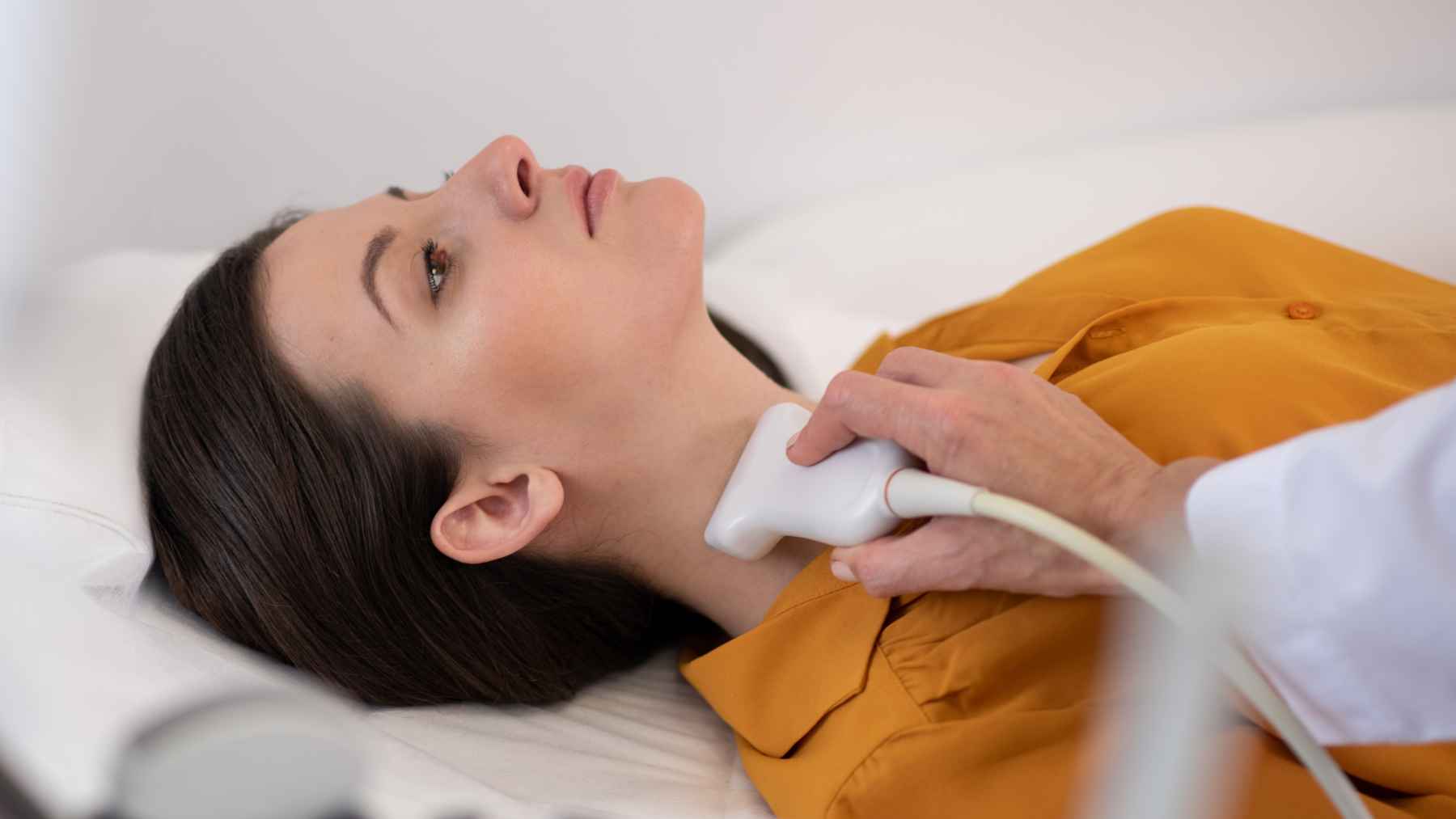
Researchers used artificial intelligence to “read” routine chest CT scans and estimate something they call “thymic health.” In large cohorts, better thymic health tracked with lower risks of death, lung cancer, and cardiovascular death, and it also lined up with stronger outcomes in patients receiving modern cancer immunotherapy.
The thymus is small but busy
The thymus sits in the chest, close to the sternum, and helps “train” T cells, the immune system’s frontline defenders that learn how to recognize threats without attacking the body’s own tissues. For decades, the common idea was that the thymus fades after puberty and becomes mostly irrelevant later in life.
These new results challenge that neat story. The data suggests thymic activity varies widely from one adult to another, and that variation may be tied to how well the immune system holds up as we age.
A new way to measure thymus health
Instead of relying on biopsies or rare lab tests, the teams built a deep-learning system that can score thymic health using routine CT images. In practical terms, that means a scan done for lung screening or cancer care might already contain information about the thymus, even if nobody is looking at it.
In the longevity and disease-risk paper, the model was developed on 5,674 CT scans and validated on 27,612 independent CT scans from two long-running cohorts. That scale matters, because it helps rule out the idea that this is just a quirky finding in a small group.
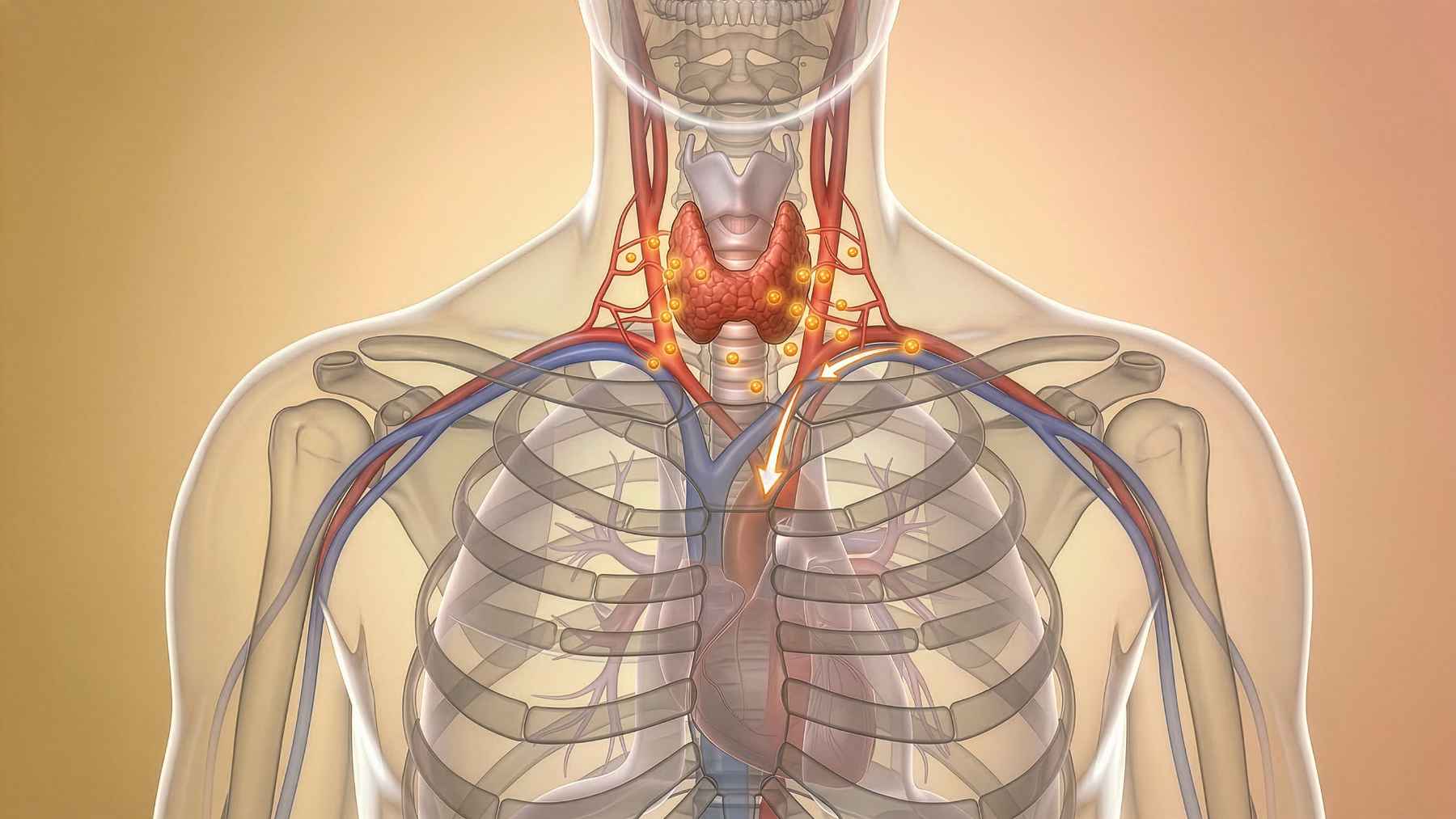
Diagram highlights the thymus gland’s position in the chest, an immune organ now linked to aging and disease risk.
What thymic health predicted in 27,612 adults
The first study combined two large prospective cohorts, the National Lung Screening Trial with 25,031 participants and the Framingham Heart Study with 2,581 participants.
Across these groups, higher thymic health was consistently linked with lower all-cause mortality, reduced lung cancer incidence, and lower cardiovascular mortality over 12 years of follow-up, even after adjusting for factors including age, sex, smoking, and other health conditions.
Some of the numbers are striking. In the National Lung Screening Trial, the 12-year mortality estimate was 13.4% in the high thymic health group versus 25.5% in the low thymic health group, with a hazard ratio of 0.49 (95% CI 0.45 to 0.53).
Cardiovascular outcomes followed a similar pattern. In the same cohort, cardiovascular-specific mortality over 12 years was 2.9% versus 7.5% (hazard ratio 0.37, 95% CI 0.31 to 0.44) when comparing high thymic health to low thymic health.
Why the lung cancer signal matters
Because one of the cohorts was built around lung cancer screening, it provides an unusually clear look at lung outcomes over time. The researchers report that higher thymic health was associated with reduced lung cancer incidence and mortality, although the paper notes that lung cancer incidence data were available over a shorter window of 6 years after randomization.
This does not mean the thymus “prevents” cancer. It does suggest that immune resilience, reflected in thymic health on imaging, may be part of the bigger story of why some people remain healthier longer even when they share similar risk factors.
The second cohort, Framingham, adds a different angle because it is deeply rooted in cardiovascular tracking. There, higher thymic health was also significantly associated with reduced cardiovascular mortality independent of age, sex, and smoking, which helps support that the finding is not limited to one single study design.
Thymus health also tracked with immunotherapy success
The second Nature study zoomed in on cancer patients treated with immune checkpoint inhibitors, the drugs designed to “release the brakes” on T cells so they can attack tumors. Using the same general approach on CT scans, the researchers quantified thymic health in a pan-cancer cohort of 3,476 patients receiving these therapies.
In patients with non-small cell lung cancer, higher thymic health was linked to lower risks of progression or death after immunotherapy. For example, in one analysis, the hazard ratio for progression-free survival was 0.65 (95% CI 0.54 to 0.77) when comparing high thymic health to low thymic health.
Overall survival moved in the same direction. The paper reports a hazard ratio of 0.56 (95% CI 0.46 to 0.68) for death when comparing high thymic health to low thymic health in the lung cancer immunotherapy cohort.
Lifestyle factors showed up in the scans
One of the most relatable parts of this research is that thymic health was not treated as a fixed trait. The authors report it varies with age and sex, and it is associated with lifestyle habits, including smoking, obesity, and low physical activity.
There were also signals linked to inflammation. In the Framingham cohort, participants with chronically elevated C-reactive protein at or above 3 mg/L across multiple measurements had substantially lower thymic health, even after accounting for sex, age, and smoking status.
Still, it is worth slowing down and asking the obvious question. Does changing lifestyle improve the thymus, or is thymic decline simply a marker of other changes happening in the body? The researchers and affiliated press materials emphasize these are observational associations, so they cannot prove cause and effect, and the imaging method is not ready for routine clinical use yet.
What to watch for next
If these results hold up, thymic health could become a useful piece of the risk puzzle. It might help identify adults who are aging immunologically faster than expected, or help clinicians think beyond tumor-only markers when selecting and timing immunotherapy.
There is also a research momentum angle here that feels very current. The paper notes growing interest in regenerative approaches and points to efforts like the ARPA for Health-funded Thymus Rejuvenation program, signaling that scientists are actively exploring whether thymic function can be preserved or restored.
For now, the most grounded takeaway is simple and surprisingly human. The immune system is not just a childhood project, and the thymus may be more like a slow-burning battery than a switch that flips off at puberty.
The study was published in Nature.